
Corneal collagen cross-linking
What is collagen cross-linking surgery?
Collagen cross-linking is a medical procedure that helps stop or slow the progression of corneal ectasia.
The most common type of corneal ectasia is keratoconus – a degenerative condition where the cornea (the clear outer layer of the eye) gradually weakens, thins and re-shapes.1–3 As the cornea helps to focus light onto the retina, any changes to its shape can cause blurred vision and problems seeing objects close-up and far away.
While the cause of keratoconus is not yet fully known, the condition tends to progress faster in younger patients. Cross-linking treatment should begin as early as possible to help prevent any further visual deterioration.
Collagen-cross linking uses a biochemical reaction to strengthen the cornea.
How does collagen cross-linking work?
Collagen cross-linking uses riboflavin (vitamin B2) eye drops and ultra-violet (UV) light to create new bonds between collagen fibres in the cornea. This results in a cornea that is stiffer and more resistant to any change in its shape.
The procedure occurs in the following steps:
- Under topical anaesthesia, your surgeon will gently remove the top layer of the cornea (the epithelium) with a soft cotton bud. This is known as the epithelium-off or epi-off protocol. The procedure can also be performed by weakening the epithelium, known as the epithelium-on protocol.
- Next, they will apply a riboflavin solution to the eye.
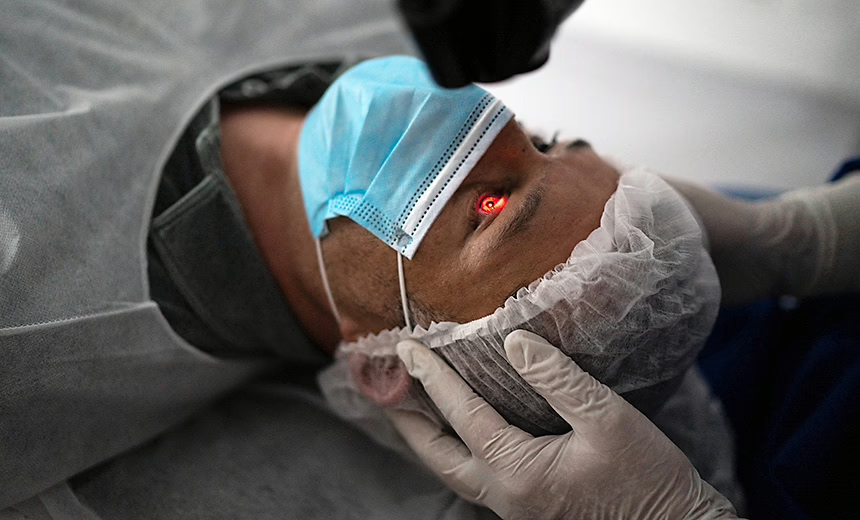
- Applying a UV light then activates the riboflavin solution as it begins to fluoresce. Note: the UV light only reaches the top layers of the eye.
- The activated riboflavin causes the collagen strands within the cornea to create new bonds, increasing its strength.
Typically, your surgeon will only treat one eye at a time. This is because there is a small risk of infection occurring.
What happens after a collagen cross-linking procedure?
Following the procedure, your ophthalmologist will place a thin bandage contact lens on your eye, where it will remain for up to three days. You will also need to apply antibiotic eye drops until the surface of your eye has healed. This helps prevent any infections from occurring. In addition, you will need to use steroidal eye drops for around five to six weeks.
What does collagen cross-linking achieve?
Collagen cross-linking aims to stabilise corneal ectasia and prevent it from getting worse. It’s important to note that it is not possible to reverse any changes that have already occurred.
How long does collagen cross-linking take?
In total, the procedure takes around one hour to complete. Cross-linking is performed as an outpatient procedure in the clinic, so patients can return home after the treatment.
Does collagen cross-linking hurt?
A local anaesthetic is applied to the eye first to minimise any pain. However, it is not uncommon to experience some mild discomfort in the immediate postoperative period. Most patients recover quickly and will be provided with oral pain relief if required.
What are the risks and complications of collagen cross-linking?
As with any surgical procedure, there is a small risk of infection. The procedure does not cause bleeding of the eye because affected corneas do not have a blood supply. The UV light is not very strong and only penetrates the cornea, not deeper structures of the eye. Riboflavin (vitamin B2) is a natural compound that is found in our diet, for example corn flakes.
How effective is collagen cross-linking?
The arrival of collagen cross-linking has given patients with keratoconus more options when it comes to the health of their cornea. Although collagen cross-linking isn’t a cure for keratoconus, it is currently the only available treatment capable of slowing down the condition. Epi-off treatment is very effective with success rates being greater than 95% in patients.1–3 The remaining patients may require a second treatment.
By slowing/preventing visual deterioration, collagen cross-linking may also delay or remove the need for a corneal transplant later down the track.
Is collagen cross-linking suitable for everyone?
Collagen cross-linking can help many patients with keratoconus. As keratoconus is a progressive condition, it is best to treat patients earlier rather than later. Children can also undergo collagen cross-linking; however, this is usually performed in an operating theatre under a general anaesthetic.
For some patients, collagen cross-linking may be less effective at stopping the progression of keratoconus. This includes cases where the cornea is too thin (usually less than 350 microns). While there isn’t an alternative to collagen cross-linking, variations of the standard epi-off technique have been developed.
Are there alternatives to collagen cross-linking?
The current answer is no – cross-linking is the only method that has been shown to stop the progression of keratoconus. Corneal transplantation (keratoplasty) is the other option and is usually reserved for advanced cases where vision has reduced considerably. Transplantation involves removing the diseased corneal tissue and replacing it with a donor cornea. This procedure has its own risks and, in some cases, the keratoconus can return after many years.
Is a Medicare rebate available for collagen cross-linking?
There is a Medicare rebate available for collagen cross-linking in patients with progressive keratoconus. This greatly improves patients’ total out-of-pocket costs. Patients can confirm the total cost with their eye surgeon or clinic – this will include the procedure fee, medications, postoperative reviews and bandage contact lens removal.
Other useful links
- Keratoconus Australia. Corneal crosslinking. Australia: Keratoconus Australia [date unknown]. Available at www.keratoconus.org.au/treatments/corneal-collagen-crosslinking/ [Accessed online 27 August 2021].
- Wollensak G. Crosslinking treatment of progressive keratoconus: new hope. Curr Opin Ophthalmol 2006;17(4):356–60.
- Hersh PS, Greenstein SA, Fry KL. Corneal collagen crosslinking for keratoconus and corneal ectasia: One-year results. J Cataract Refract Surg 2011;37(1):149–60.
The information on this page is general in nature. All medical and surgical procedures have potential benefits and risks. Consult your ophthalmologist for specific medical advice.
Date last reviewed: 2026-01-29 | Date for next review: 2028-01-29
